Mark K. Setton, D.Phil
Paul Min, Ph.D
Anthony Arciero, Ph.D
THE INNER PANDEMIC: IS IT UNSTOPPABLE?
THE PROBLEM
- A staggering 44% of teenagers in the US are presently experiencing “disabling episodes” of depression or anxiety. [1]
- The scale of the “inner pandemic” defies traditional approaches to treatment. US schools and universities are struggling to deal with students at high risk, let alone those merely needing support.
- Leading figures in the field of psychiatric epidemiology working on depression prevention have drawn attention to the urgent need for a “prevention first” approach. The COVID-19 pandemichas taught us the same lesson. According to the “depression prevention” group,
Despite substantial investments in the treatment of major depressive disorder, especially antidepressant medications and cognitive behavioral therapy, epidemiological data do not indicate that depression burden… has decreased in recent decades. [2]
That finding was before COVID-19. Depression rates among youth have nearly doubled during the last three years.
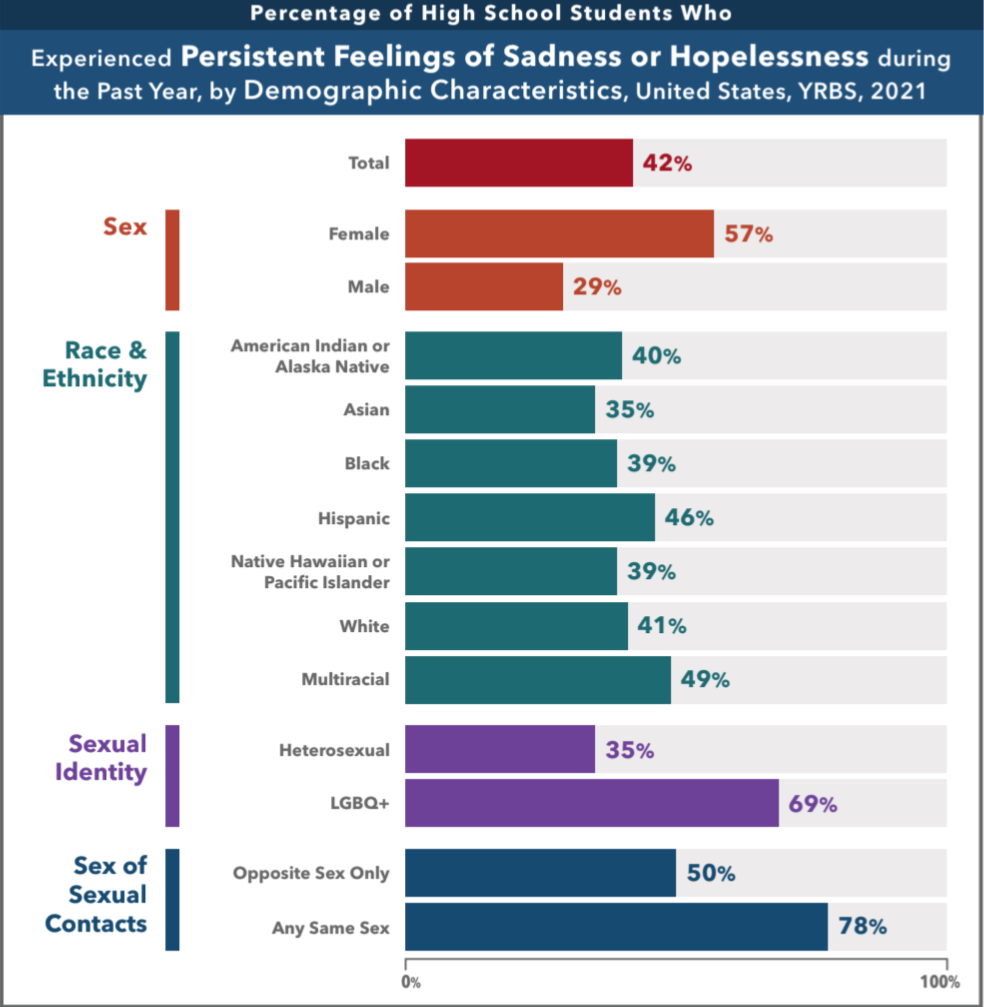
Source: CDC, Youth Risk Behavior Survey (YRBS), 2021.
NEW SOLUTIONS
Traditional approaches are failing to make a dent in what has become a new noncommunicable disease pandemic.
We urgently need innovative solutions that are both evidence-based and scalable.
- An evidence-based solution
In the US, youth depression rates, especially among females, began to jump in 2010, and had doubled by 2019. [3] Surprisingly, very few systematic attempts have been made to analyze the origins of the problem. [4]
We cannot fight the “inner pandemic” without first uncovering its causes. Thanks to an explosion of new studies, especially in the fields of neuropsychiatry and physiology, by scientists in both Asia and the West, evidence is accumulating that the depression epidemic may largely be a side-effect of rapid modernization. More specifically, it appears to be rooted in biological as well as psychosocial dysfunctions, closely related to changes in lifestyle. [5] This could be a key reason why previous interventions, heavily inclined towards the psychosocial side of the spectrum, and less towards physiological lifestyle changes, have had a small impact. [6]
https://www.pursuit-of-happiness.org/psychobiotics-2/ A remarkable example of such a blind spot is the relationship between the microbiome and psychological well-being. In 2012, Ted Dinan and John Cryan first introduced the concept of Psychobiotics, certain species of human gut bacteria that produce key neurotransmitters such as GABA, serotonin and BDNF, and suggested that they possess antidepressant and anxiolytic properties. [7]
We now know that the decline in consumption of whole foods, such as fiber-rich fruit and vegetables, the very foods that Psychobiotics feed upon, is directly related to gut dysbiosis. The shift from whole foods to processed foods has thus become a key suspect in the hunt for the roots of the inner pandemic. [8]
As with many inside jobs, a group of outsiders is involved too. We have discovered that physical exercise generates large amounts of BDNF, a neurotransmitter which is now recognized as playing a key role, at least equal to serotonin, in mood modulation. A third discovery related to the biology of well-being is that screen time, which now averages about 7.7 hours a day among teenagers in the US, not only reduces face-to-face contact, and along with it, production of the “love hormone” oxytocin, but impacts circadian rhythms and sleep cycles. [9]
Such discoveries indicate that any intervention aimed at tackling the depression pandemic needs to target concrete education and guidance on biological as well as psychosocial life skills, including nutrition, exercise, sleeping habits, and “screen hygiene.”
- A scalable solution
Recent advances in the fields of peer support and online learning are transforming perceptions regarding the scalability of interventions.
o Peer support
According to an exhaustive review by Mental Health America,
Both quantitative and qualitative evidence indicate that peer support lowers the overall cost of mental health services by reducing re-hospitalization rates and days spent in inpatient services, increasing the use of outpatient services. Peer support improves quality of life, increases and improves engagement with services, and increases whole health and self-management. [10], [11]
https://www.pursuit-of-happiness.org/keskps/ Peer support could moreover be a vital tool in pandemic mitigation for the following reasons:
-
Scalability: By definition, peer support is a nearly unlimited resource.
-
Accessibility: Most victims of depression fail to engage with professionals for economic or personal reasons. On top of providing voluntary services, peer supporters are often more readily accessible, as they share work or leisure spaces with support recipients.
-
Trainability: Peer supporters can play certain roles with minimal training. They can perform two critical tasks that can be taught relatively easily:
-
Active listening. Through active listening, a practice regarded as a powerful catalyst of successful relationships, peer supporters provide a sense of companionship which facilitates increased engagement.
-
Recognizing emotional status and intention to the degree necessary for appropriate “signposting.”
For example:
o At-risk individuals can be encouraged to contact emergency services and apply for urgent care as well as guided towards appropriate community engagement and educational programs.
o Moderately or mildly depressed / anxious individuals can be steered towards appropriate community engagement and educational programs.
o Online Learning Platforms
A new generation of sophisticated online learning platforms now makes it possible to provide engaging, low-cost educational programs, on an unprecedented scale, in order to:
-
train peer supporters
-
provide education on critical life skills to recipients of peer support.
CONCLUSION
- Due to the scale of the “inner pandemic,” preventive strategies must become a priority.
- Expert consensus in the field of depression prevention now recognizes that existing preventive strategies are not sufficient. Novel strategies are needed both in terms of methodology and scalability
- In terms of methodology, evidence is accumulating that the depression epidemic may be rooted in biological as well as psychosocial dysfunctions, closely related to changes in lifestyle. Educational programs relating to lifestyle, and specifically evidence-based life skills, would thus be a priority.
- In terms of scalability, peer support, based on systematic training, is widely recognized to be highly effective. Training for peer supporters, as well as the signposting of educational programs for recipients of peer support, is now eminently scalable with the use of online learning platforms.
- Online educational programs aimed at peer support training as well as end users, and focused on the cultivation of evidence-based life skills, are a cost-effective approach to tackling the depression pandemic, especially for underrepresented communities.
RECOMMENDATIONS
In 2021-2022 the Pursuit of Happiness team completed a pilot intervention at the University of Strathclyde, which combined an online educational program focused on life skills conducive to depression prevention, with an onsite peer support component. The intervention had a significant impact on measures of depression, overall psychological well-being, and self-efficacy. The participants described the life-changing effect of connecting with their peers, feeling heard and understood, and gaining specific knowledge and skills to build their well-being. [12], [13]
As a next step, we would thus recommend a larger controlled intervention in the US, especially aimed at underrepresented communities, in order to replicate the results.
[1] New CDC data illuminate youth mental health threats during the COVID-19 pandemic (https://www.cdc.gov/media/releases/2022/p0331-youth-mental-health-covid-19.html).
[2] Ormel, J., Cuijpers, P., Jorm, A., & Schoevers, R. A. (2020). What is needed to eradicate the depression epidemic, and why. Mental Health & Prevention, 17, 200177, p. 1. https://doi.org/10.1016/j.mhp.2019.200177
[3] See the shocking figures illustrating the sudden rise of youth depression around 2010 at https://www.childstats.gov/americaschildren/health_fig.asp#health4a
[4] We have recently seen much discussion about the psychosocial impact of COVID-19, which triggered a secondary jump in both depression and anxiety, but not about why those rates began to steeply climb a decade earlier.
[5] Hidaka, B. H. (2012). Depression as a disease of modernity: Explanations for increasing prevalence. Journal of Affective Disorders, 140(3), 205–214. https://doi.org/10.1016/j.jad.2011.12.036
[6] Ormel, J., Cuijpers, P., Jorm, A., & Schoevers, R. A. (2020). What is needed to eradicate the depression epidemic, and why. Mental Health & Prevention, 17, 200177. https://doi.org/10.1016/j.mhp.2019.200177
[7] Dinan, T. G., Stanton, C., & Cryan, J. F. (2013). Psychobiotics: A novel class of psychotropic. Biological Psychiatry, 74(10), 720–726.
[8] Simpson, C. A., Diaz-Arteche, C., Eliby, D., Schwartz, O. S., Simmons, J. G., & Cowan, C. S. M. (2021). The gut microbiota in anxiety and depression – a systematic review. Clinical Psychology Review, 83, 101943. https://doi.org/10.1016/j.cpr.2020.101943
[9] Nagata, J. M., Cortez, C. A., Cattle, C. J., Ganson, K. T., Iyer, P., Bibbins-Domingo, K., & Baker, F. C. (2022). Screen Time Use among US adolescents during the COVID-19 pandemic. JAMA Pediatrics, 176(1), 94. https://doi.org/10.1001/jamapediatrics.2021.4334
[10] https://www.mhanational.org/sites/default/files/Evidence%20for%20Peer%20Support%20May%202018.pdf
[11] See also Pfeiffer, P. N., Heisler, M., Piette, J. D., Rogers, M. A. M., & Valenstein, M. (2011). Efficacy of peer support interventions for depression: A meta-analysis. General Hospital Psychiatry, 33(1), 29–36. https://doi.org/10.1016/j.genhosppsych.2010.10.002
[12] See enclosed report on the “Hear to Listen” initiative at the University of Strathclyde.
[13] See related motion by UK House of Parliament at https://edm.parliament.uk/early-day-motion/59612?trk=public_post_embed_feed-article-content.